Introduction
The two circulations in the body
Blood vessels
Function
Structure
Tissue fluid
So a blood vessel entering the liver or kidneys would be an artery. A blood vessel leaving the liver or kidneys would be a vein.
he liver attribute is hepatic ( for example, the working cell unit in the liver is the hepatic cell), while the kidney attribute is renal (for example, renal failure). So what would the blood vessel entering the liver be called?
…pressing question.
…pressing on.
…
…the hepatic artery! Same principle applies to the rest: the hepatic vein, the renal artery and the renal vein.
There’s a catch (welcome to biology). In the case of the blood vessels leaving or entering the lungs, the rules are reversed. The pulmonary vein carries oxygenated blood to the heart, while the pulmonary artery carries deoxygenated blood into the lungs.
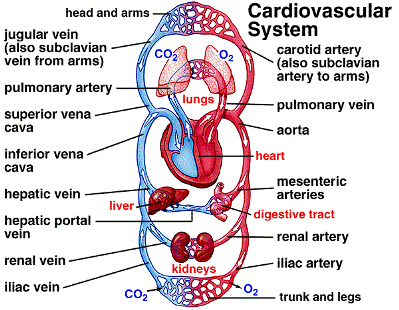
You also need to learn the blood vessels entering and leaving the heart.
- The aorta is the main artery which carries oxygen-rich blood to the rest of the body.
- The coronary arteries supply blood to the heart itself (and they are the affected arteries in coronary heart disease).
- The superior vena cava and the inferior vena cava bring deoxygenated blood from the upper half of the body, and the lower part of the body respectively.
It’s all really logical… apart from the bit on the lungs.
Blood vessels
There are 4 types of blood vessels: arteries, arterioles, capillaries and veins. Each type has a different function…
