Alzheimer’s disease
Hearing, vision and memory loss
Alzheimer’s disease
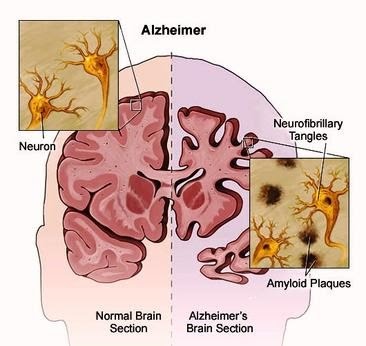
Alzheimer’s disease is the most prevalent type of dementia. Dementia is a disease affecting the brain, caused by an interplay of genetic and environmental factors over time. Age is the main risk factor for developing Alzheimer’s disease.
Neurons die gradually as Alzheimer’s disease progresses over several years, due to buildups of otherwise safe proteins including amyloid and tau. Amyloid forms plaques between neurons while tau forms tangles inside them. These structures result in the death of brain cells.