Risk factors and causes of cancer
Diagnosis and treatment
Risk factors and causes of cancer
Apart from specific, easily identifiable pathogens such as bacteria or viruses which can cause disease, another major cause of disease is lifestyle. Lifestyle includes the choices that we make in regards to our food, drink, whether we smoke or use drugs, certain jobs we do, even the place where we live.
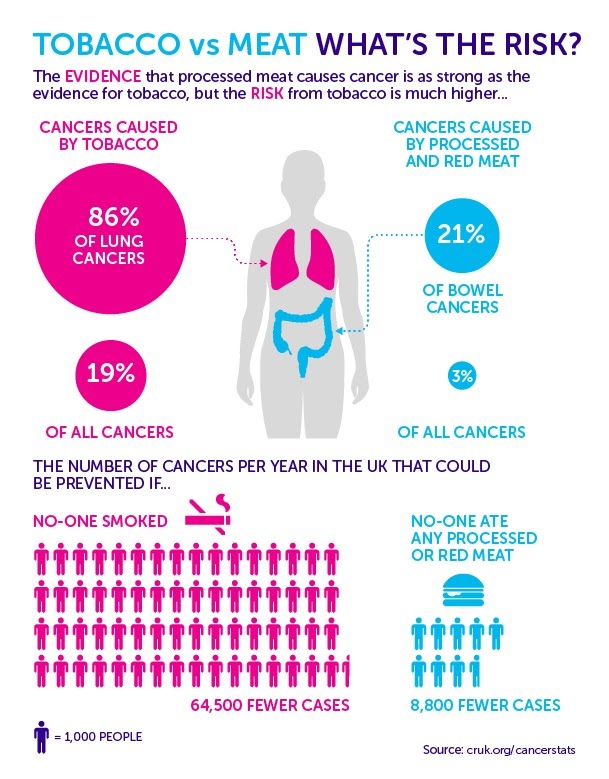
The way we can measure the impact of certain lifestyle choices is by knowing risk factors. Certain diseases like cancer and coronary heart disease are associated with certain risk factors, such as smoking and obesity. On the flip side, changes in lifestyle are also associated with a decrease in risk of contracting these diseases.
A key risk factor for bowel cancer is diet. Specifically, consumption of processed and red meats has been positively correlated with the incidence of bowel cancer, while consumption of fibre from whole grains, fruit, vegetables and enough water has been negatively correlated with bowel cancer, while consumption of fiber from whole, fruits, vegetables and enough water has been negatively correlated with bowel cancer.
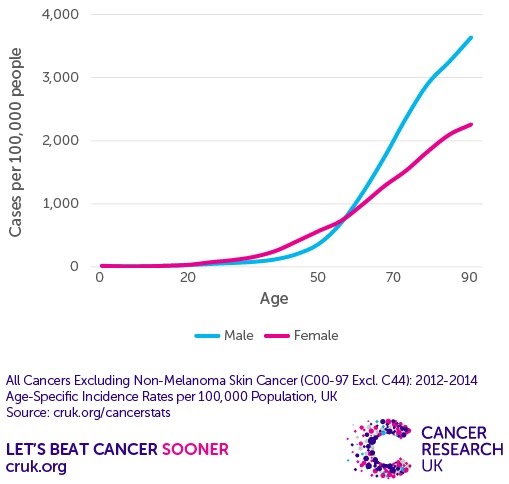
Cancer risk factors include heredity, ageing, different types of radiation such as UV and cosmic rays, carcinogens, air pollution and viruses (unlike HIV and influenza viruses which lead to communicable disease, some viral infections can be associated with non-communicable disease such as cancer, e.g. HPV and cervical cancer, hepatitis B and liver cancer).
You should be able to analyse graphs showing specific risk factors, such as age, sex or smoking against the incidence of disease such as lung cancer or heart disease….
