Introduction
fMRI
CT
PET
EEG
Introduction
There are multiple techniques available in research and medicine to study the brain for various purposes including diagnosis and psychology research.
fMRI
Functional magnetic resonance imaging (fMRI) is used more so in research than medicine, and gives a picture of brain activity based on increased blood flow correlated with neural activity.
This is based on the knowledge that wherever in the brain higher activity takes place, an increase in blood will take place. This creates a gradient between the deoxygenatedhaemoglobin in the blood and the oxygenated haemoglobin in the blood. Because oxygen in haemoglobin is bound to the iron present, deoxygenated haemoglobin will have unbound iron ions. These respond magnetically to the magnetic field applied during the procedure.
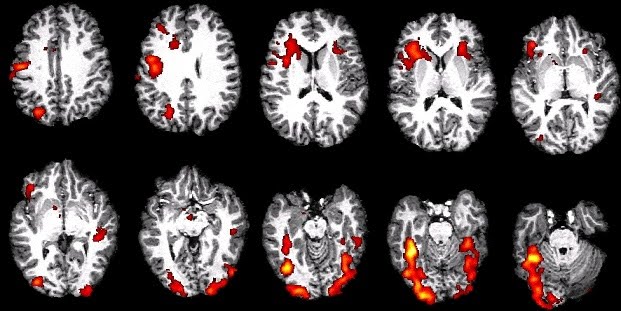
By processing the data obtained through the procedure (which involves picking up the blood flow differences via magnetic fields and radio frequency waves), a map of brain activity emerges. Within an experiment, this is cross-referenced with a control state, whether for a patient or group of participants in a study, in order to interpret the data.
Limitations of fMRI include noise which interferes with the signals e.g. from heat in the vicinity of the scanner, movement of the participant or system noise coming from the hardware, and statistics needed to make use of the raw data. Sometimes the statistics used was not robust enough to distinguish between real differences in brain activity and noise. Famously, the fMRI data of a dead salmon was used to show real differences…….
