Haemoglobin (WJEC)
Blood components
Erythrocytes
Haemoglobin
Myoglobin
Foetal haemoglobin
Blood components
Blood is fun! Blood is to body as the Thames is to London, although I sure hope slightly cleaner…
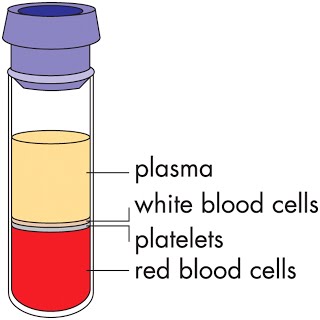
Blood is roughly split into the plasma and blood cells including erythrocytes and leucocytes (neutrophils, eosinophils, monocytes, lymphocytes). Plasma is the solution that blood cells are found in, and as such acts as their extracellular matrix. For skin cells for example, the extracellular matrix is formed of collagen, so it’s different to have it essentially a liquid like plasma. Plasma is a water solution containing proteins, sugars, clotting factors (as well as platelets involved in clotting), hormones, electrolytes, carbon dioxide and oxygen.
Erythrocytes
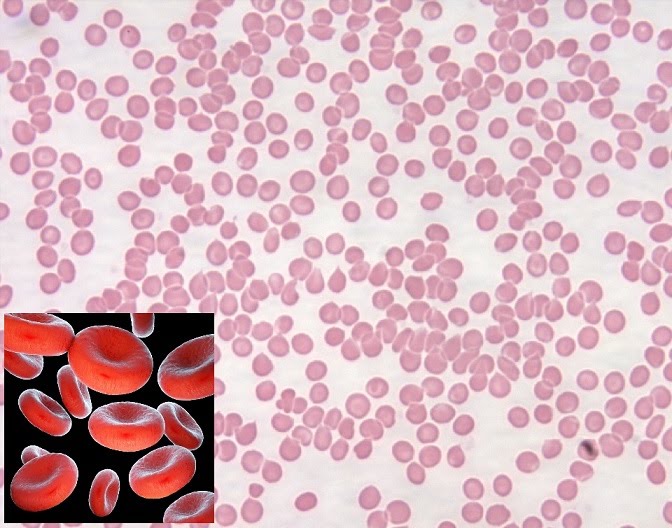
Erythrocytes are red blood cells/RBC (and also the most common blood cells) carrying haemoglobin around the body. Haemoglobin can bind and release oxygen and is central to aerobic respiration.
Haemoglobin
Carbon dioxide and oxygen are transported in the blood under different conditions. Carbon dioxide is more soluble than oxygen, so some of it is directly present in the blood plasma. It can also be present as bicarbonate ions which increase blood acidity and signal if there is too much CO2 in the blood and not enough O2.
inally, both CO2 and O2 can bind to haemoglobin which is present in red blood cells. Its function is the oxygenation of tissues, as oxygen is central to aerobic respiration, the metabolic process of creating chemical energy for all cell functions. Its smaller cousin, myoglobin, stores rather than transports oxygen in the body, and instead of being found in the blood, resides in muscle tissue. It only has one haem group so can only bind one oxygen molecule, while haemoglobin binds up to 4.
Haemoglobin is a type of protein. It is present in many varied organisms on our planet, and has a similar chemical structure in all of these organisms. In humans, haemoglobin is found in red blood cells. Haemoglobin’s function is….



